Sarampión: signos y síntomas
Obtenga más información sobre qué es el virus del sarampión y cómo se propaga
February 19, 2025
¿Qué es el sarampión?
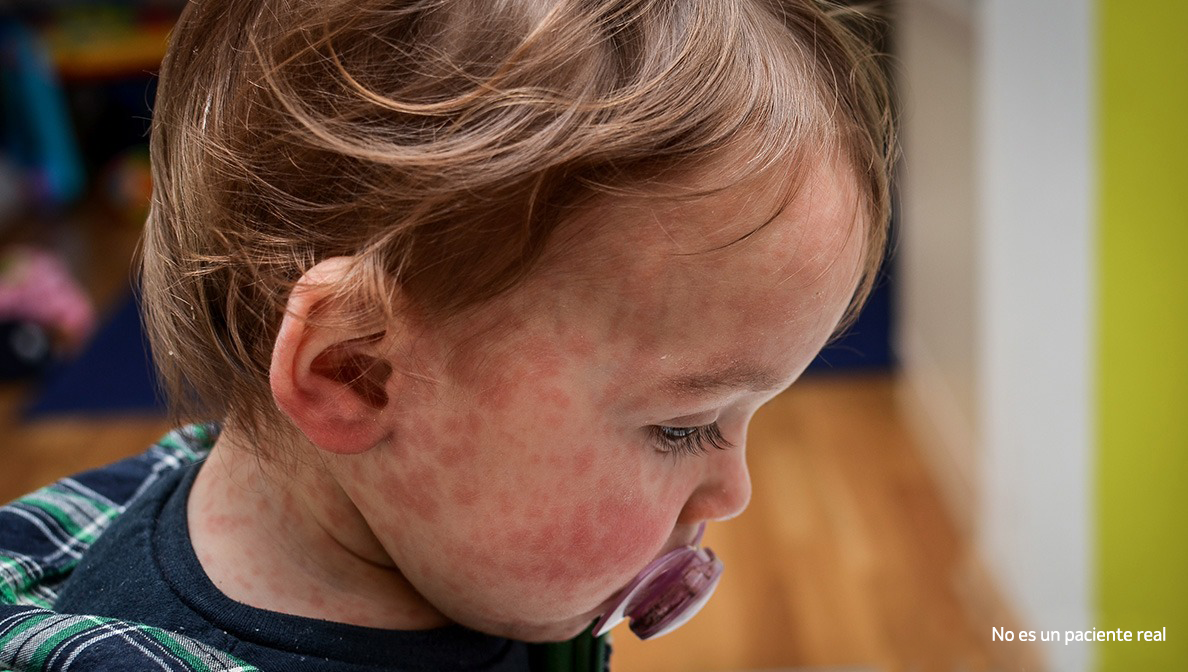
El sarampión es una enfermedad viral altamente contagiosa que puede afectar a personas de todas las edades, pero es más común en los niños. El virus vive en la mucosidad de la nariz y en la garganta de una persona infectada.
El sarampión se propaga por el aire cuando una persona infectada tose o estornuda. Los síntomas aparecen entre 7 y 14 días después del contacto con el virus.
Los síntomas comunes del sarampión incluyen los siguientes:

Fiebre alta
(puede subir repentinamente a más de 104 °F)

Tos

Moqueo

Ojos rojos y llorosos
(conjuntivitis)
Manchas en la boca
(2-3 días después de que comiencen los síntomas)

Erupción
(3-5 días después de que comiencen los síntomas)
Cómo se propaga el sarampión
El sarampión puede ser grave y causar complicaciones
- Aproximadamente 1 de cada 5 personas no vacunadas en los EE. UU. que contraen sarampión se hospitalizan.
- Hasta 1 de cada 20 niños con sarampión contrae neumonía, que es la causa más común de muerte por sarampión en niños pequeños.
- Aproximadamente entre 1 y 3 de cada 1,000 niños que se infectan de sarampión morirán por complicaciones respiratorias y neurológicas.
Brotes de sarampión
Antes de la disponibilidad de la vacuna en 1963, se estima que entre 3 y 4 millones de estadounidenses contraían sarampión cada año, y se calcula que 48,000 personas en Estados Unidos se hospitalizaban y se producían aproximadamente entre 400 y 500 muertes al año.
Cuando usted se contagia de sarampión, hasta el 90% de las personas a su alrededor que no estén vacunadas también se infectarán.
En los Estados Unidos, los casos de sarampión pueden originarse en viajes internacionales, ya que la enfermedad sigue siendo común en muchas partes del mundo. Por lo general, 2 de cada 3 viajeros con sarampión son estadounidenses no vacunados que reingresan al país.
Como lo demuestran los brotes recientes en todo el país, el sarampión se puede propagar rápidamente y las personas infectadas pueden contagiar a personas que no son inmunes.